Achieve a seamless RCM cycle in medical billing with our experts and focus on delivering quality care to patients. Similarly, we offer healthcare revenue cycle management services to medical practices in the US. Our RCM experts help providers to optimize practice revenue.

Our medical billing professionals follow a tailored approach to drive maximum revenue for your healthcare practice. As a result, you get timely and accurate reimbursements. To maximize profit generation, we ensure clean claim submissions to avoid revenue losses. Also, our experts help providers get financial success across the entire revenue cycle spectrum. Further, we deliver end-to-end RCM management services to boost cash collections and minimize costs. As a result, it significantly improves the financial health of your medical practice.
Easy Claim Med offers tailored solutions based on enhanced revenue cycle methods for medical practices of all sizes.
We offer customized healthcare revenue cycle management solutions to boost financial outcomes and reduce accounts receivable. In addition, our RCM billing services help increase the reimbursement rates and charge capture. Therefore, medical practices are able to achieve financial integrity and drive competitive edge. We optimize the end-to-end revenue cycle to improve net revenue and reduce claim denials. So, medical practices of all sizes get tailored solutions based on enhanced revenue cycle methods.
It is the process of balancing and managing the financial operations of a healthcare organization. It further streamlines billing operations, ensuring providers receive timely reimbursement for medical services rendered.
It improves your financial health by reducing claim rejection, accounts receivable days, and ensuring regulatory compliance. Furthermore, an effective RCM strategy helps increase the overall collections.
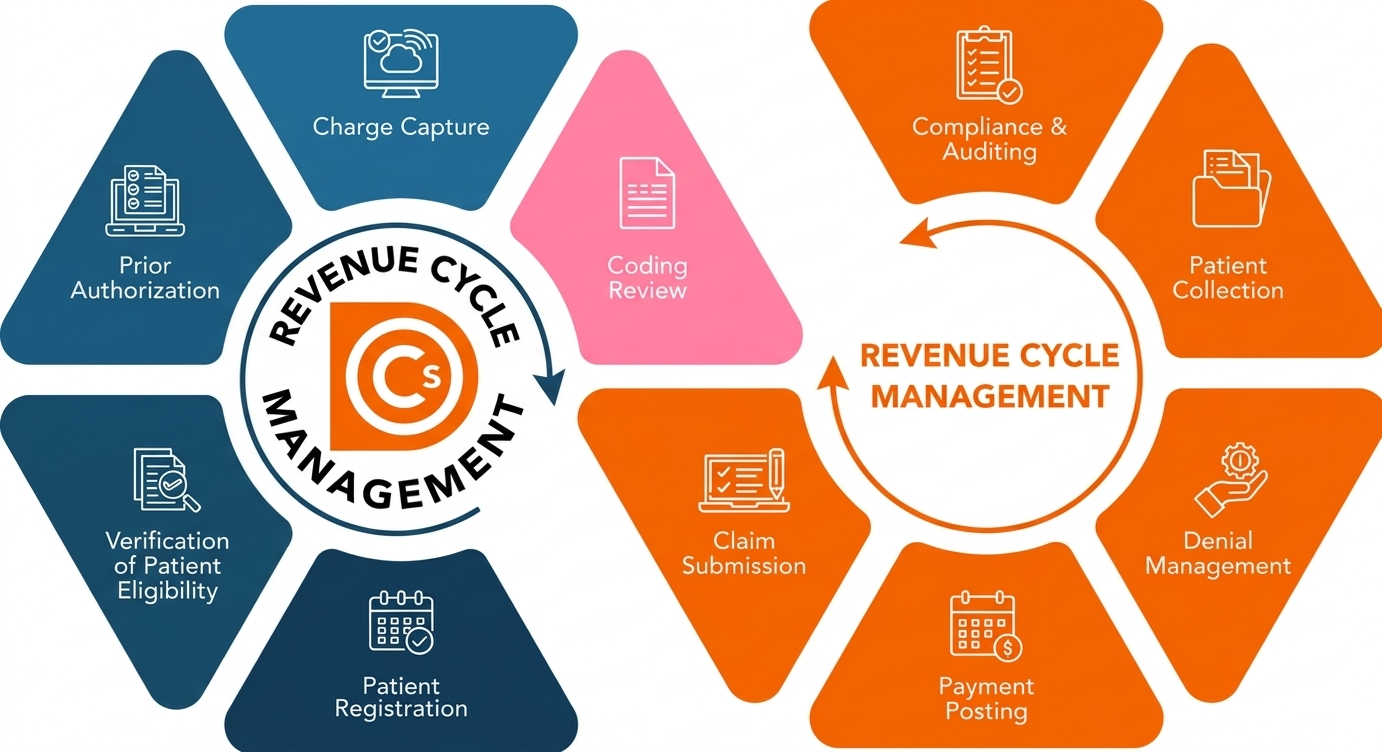
RCM services include patient registration, insurance eligibility verification, charge capture, claims submission, denial management, payment posting, accounts receivable follow-up, and reporting