Our provider credentialing services in USA enable healthcare providers to save time and focus on core areas. Similarly, we help you simplify the credentialing and enrollment process. In addition, it enables providers to prevent reimbursement delays and use resources wisely.

Our provider enrollment and credentialing services help providers to get enrolled with payers like Medicare, Medicaid, and commercial plans. Additionally, we carefully submit your documents to payers and help become an in-network provider. As a result, you are able to get payments from all the insurance carriers. Since credentialing is an on-going process, we help both new and old medical practices to expand their network. Our medical credentialing services help new providers to begin their practice while complying with the rules. Also, we help healthcare providers to maintain their CAQH profile and complete the re-credentialing process.
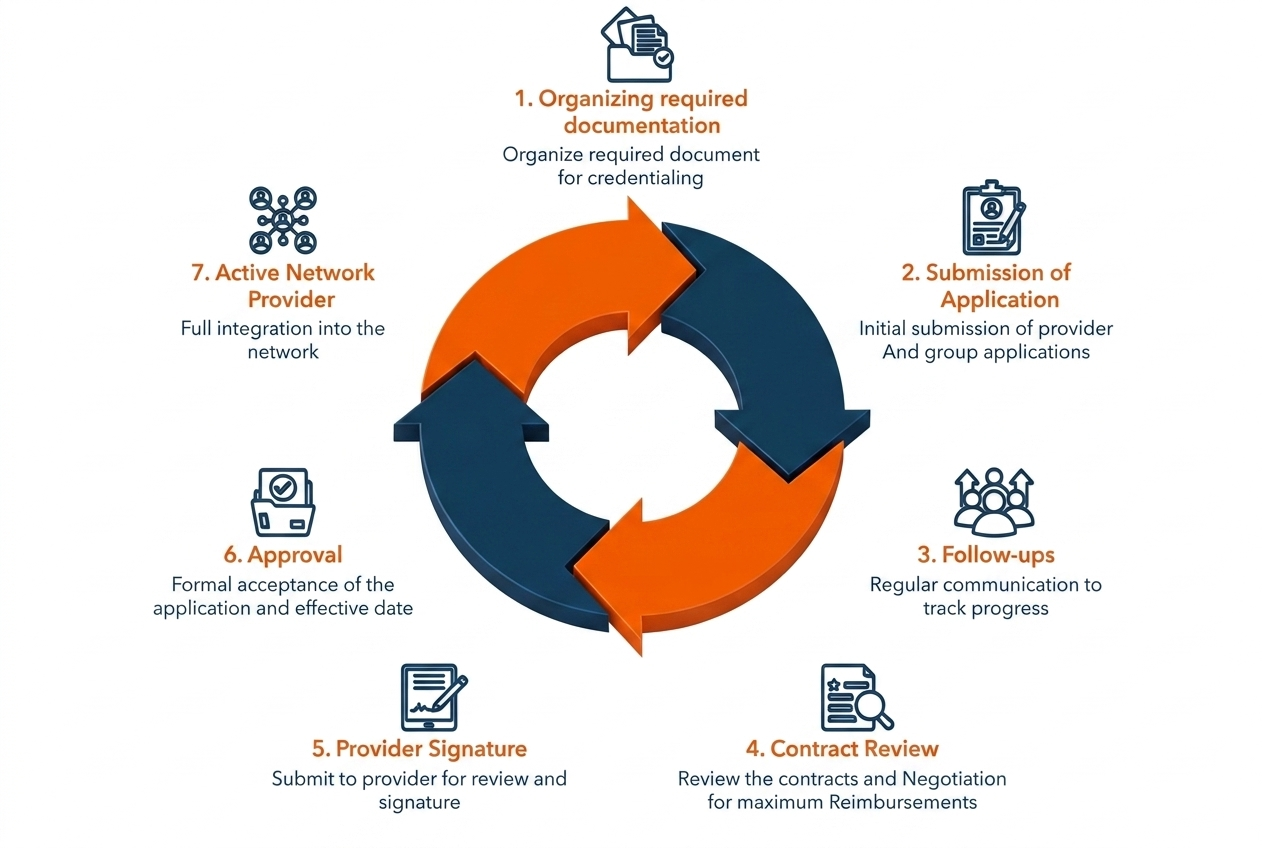
Provider credentialing is a process in which the credentialing committee analyzes whether the education, medical training, certifications, and licensing are authentic. Likewise, it ensures that the provider is eligible to render medical services and receive reimbursement.
Credentialing is not a one-time process. It needs renewal after 2 years, but the renewal date may vary according to organizational policies and the payer’s requirements.
Credentialing is important for healthcare providers because it helps them deliver medical care and receive accurate payment for the services rendered.